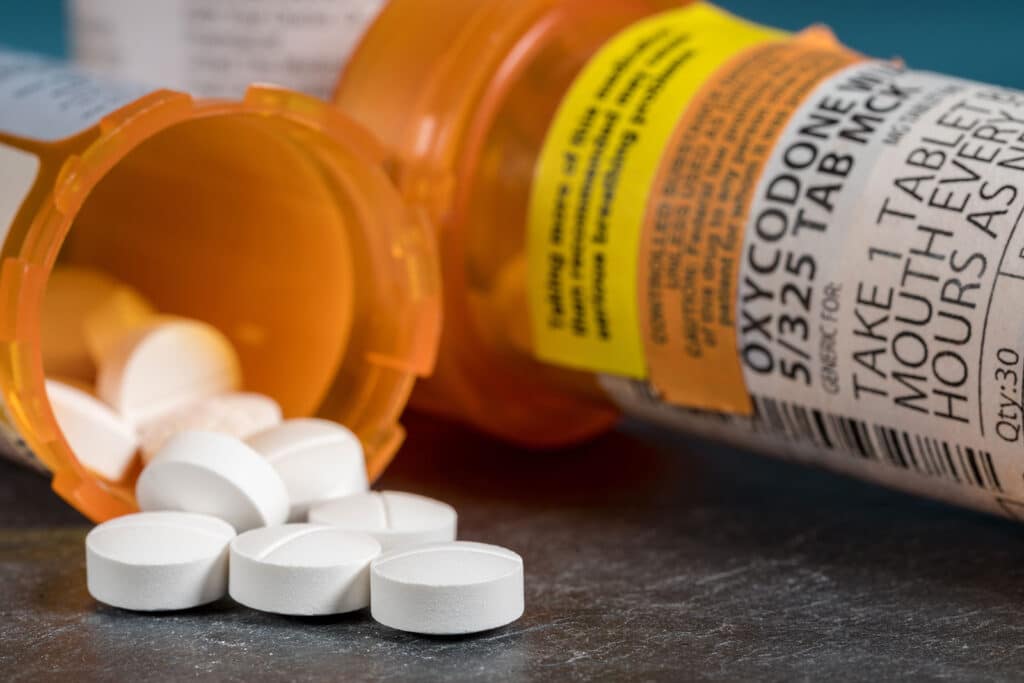
In the United States, nearly one in five adults filled a prescription for opioids in the past year. These medications can help with severe pain, but how long do they linger in your body? And what happens once they’re gone?
The answer isn’t simple. A dose of oxycodone might clear from your bloodstream in under a day. However, it can still be detected in urine tests for up to four days, and in hair tests for as long as 90 days.
Whether you’re using pain medication as prescribed or concerned about possible opioid addiction, knowing how long it stays in your system is important. It’s pivotal for your health and safety.
Understanding Pain Pills and Their Effects
People often think of pain pills as prescription opioids like oxycodone or hydrocodone, which are medications that bind to opioid receptors in the brain to block pain signals.
However, pain medication is a much broader class of drugs, and not all carry the same risks, side effects, or detection times.
Here’s a breakdown of the main types and how they work:
Non-Opioids
Medications like acetaminophen (Tylenol) or NSAIDs such as ibuprofen (Advil) and naproxen (Aleve) are used for mild to moderate pain and inflammation. They have a short half-life, often leaving the body within 24 hours, and rarely show up in standard drug testing.
Adjuvant Pain Medications
Certain antidepressants (such as amitriptyline) and anticonvulsants (such as gabapentin) are prescribed for nerve-related pain. They aren’t usually screened for in urine tests, but they can remain in your system for several days, depending on your metabolic rate.
Muscle Relaxants
Often prescribed for muscle spasms, these act on the central nervous system to ease tension. They’re generally detectable for one to two days in urine tests, but may cause lingering drowsiness beyond that.
Opioids
This includes natural opioids derived from the poppy plant (like morphine and codeine), semi-synthetic opioids (like oxycodone, hydrocodone, and oxymorphone), and synthetic opioids (like fentanyl and methadone).
Short-acting opioids may be eliminated within a couple of days, while long-acting opioids can be present for a longer period. Chronic or high-dose use often extends the detection window significantly.
Each type is prescribed for different situations, from post-surgery recovery to managing chronic pain. They all have potential side effects, and opioids, in particular, carry a higher risk of opioid use disorder (OUD), which currently affects 2.1 million individuals in the United States.
Understanding the type of medication you’re taking is the first step toward knowing how long it might stay in your system and when withdrawal symptoms could begin if you stop.
Factors Affecting How Long Opioids Stay in Your System
There’s no single “expiration clock” for pain pills in the body. Two people could take the same type of opioid, at the same dose, and have completely different detection times.
That’s because a mix of biological and lifestyle factors influences how your body processes the medication and its metabolites.
1. Dosage and Frequency of Use
The more you take, and the more often you take it, the longer it can take for your body to fully eliminate the drug. Higher doses increase the amount of active drug and metabolites in your system, extending the detection window.
Long-term or heavy opioid use often leads to the drug being stored in body tissues, which can slowly release over time.
2. Type of Medication
Short-acting pain relievers, such as immediate-release oxycodone or codeine, are typically cleared faster than long-acting opioids like extended-release oxycodone (OxyContin) or methadone.
Some synthetic opioids, especially fentanyl, may leave the bloodstream quickly but remain in fatty tissues, where they can be slowly released.
3. Individual Factors
Your metabolic rate, hydration levels, age, body weight, and overall health all affect how long medications linger. Healthy liver and kidney function allows your body to filter and process drugs more efficiently.
4. Method of Administration
Whether a medication is swallowed, injected, or absorbed through a patch changes how quickly it’s absorbed, processed, and cleared. For example, transdermal fentanyl patches release the drug steadily, often prolonging the length of time it remains detectable.
5. Other Medications and Substances
Mixing pain pills with other substances, including alcohol, benzodiazepines, or certain antidepressants, can interfere with how the body processes them. This may increase side effects and lengthen elimination times.
Detection Windows for Common Pain Medications
How long pain pills remain detectable depends not only on the drug itself but also on the testing methods used.
Different tests look for different markers. Some detect the drug directly, while others detect metabolites left behind after your body processes it.
Here’s a general guide to detection times for some of the most common prescription opioids and related medications. Keep in mind these are average estimates; your individual factors, frequency of use, and type of opioid can shift the timeline.
| Medication | Urine Tests | Blood Tests | Saliva Tests | Hair Tests |
| Oxycodone (OxyContin, Percocet) | 3–4 days | Up to 24 hours | 1–2 days | Up to 90 days |
| Hydrocodone (Vicodin, Norco) | 2–4 days | Up to 24 hours | 1–2 days | Up to 90 days |
| Codeine | 1–3 days | Up to 24 hours | 1–2 days | Up to 90 days |
| Fentanyl (synthetic opioid) | 1–3 days | Up to 12 hours | 1–2 days | Up to 90 days |
| Methadone (long-acting synthetic opioid) | 7–10 days | Up to 48 hours | 1–4 days | Up to 90 days |
| Morphine (natural opioid) | 2–3 days | Up to 24 hours | 1–2 days | Up to 90 days |
Why the Differences?
- Urine tests are the most common in the workplace and rehab drug screens because they’re easy, affordable, and have a reasonable detection window for most drugs.
- Blood tests are less common for routine screening because the amount of time drugs remain in the bloodstream is relatively short. They’re often used in accident investigations or medical settings to measure a drug’s effects in real time.
- Saliva tests detect recent drug use and are easy to administer, but have a narrower detection window.
- Hair tests can reveal a history of substance abuse over a longer period (up to 90 days), but won’t reliably detect very recent use.
These ranges also shift based on short-acting opioids versus long-acting opioids. For example, a single dose of short half-life codeine may be gone from urine within a couple of days, while long-acting opioids like methadone may remain for over a week.
Short-Term and Long-Term Effects of Pain Pills Use
Pain pills can provide life-changing pain relief, but they also affect more than just discomfort levels.
Even short-term use can trigger side effects such as drowsiness, slowed breathing, constipation, and reduced coordination. High doses increase the risk of overdose. With prolonged or high-frequency use, the body adapts, leading to tolerance and opioid use disorder.
Long-term effects may include persistent constipation, hormonal changes, weakened immune function, liver or kidney strain, and heightened sensitivity to pain. Mental health can also suffer, with depression, anxiety, and intense cravings becoming part of the cycle.
Furthermore, chronic opioid use can change how the body processes medications, sometimes lengthening detection windows in drug testing. These changes also make quitting harder and riskier if done without medical guidance.

Withdrawal and Why It Happens
When the body becomes used to a steady supply of pain pills, particularly prescription opioids, it adapts by adjusting brain chemistry and how opioid receptors function. Stop taking the medication suddenly, and your system scrambles to rebalance, triggering withdrawal symptoms.
For short-acting opioids like codeine or hydrocodone, symptoms can begin within 6–12 hours after the last dose. For long-acting opioids like methadone, it might take 24–36 hours before they appear.
Common symptoms include:
- Muscle aches
- Sweating
- Nausea
- Anxiety
- Insomnia
- Intense cravings
While opioid withdrawal is rarely life-threatening, it can be deeply uncomfortable, and relapse often occurs when people try to quit without support.
The safest approach is a medically supervised detox, where healthcare providers can monitor symptoms, manage discomfort, and reduce the risk of complications.
Detoxing from Pain Pills Safely
Quitting pain pills without medical help, which is often called going “cold turkey,” can be quite risky. Not only can withdrawal symptoms be intense, but the sudden loss of opioid effects may trigger severe cravings and rapid relapse.
A medical detox offers a safer path. In a supervised setting, healthcare providers can monitor vital signs, ease discomfort with approved medications, and address complications as they arise. For some, medication-assisted treatment (MAT) with drugs like buprenorphine or methadone can reduce cravings and make the process more manageable.

The detox timeline depends on the type of opioid, half-life, and frequency of use. Short-acting opioids may clear in a few days, while long-acting opioids or chronic use may require a longer period for the body to adjust.
Even after the drug is physically gone, emotional and psychological effects can persist, which is why a detox is often the first step in a larger treatment plan.
Some people benefit from inpatient care, where they can focus entirely on recovery in a structured, supportive environment. Others choose outpatient programs, which allow them to maintain work, school, or family responsibilities while still receiving therapy and medical oversight.
Effective treatment often combines counseling, behavioral therapy, peer support, and, when appropriate, ongoing medication-assisted treatment.
Final Thoughts
Recovery from opioid addiction or dependence doesn’t end with detox. The real work begins in the days and weeks that follow, when the body and mind adjust to life without pain pills. That’s when having the right treatment programs and support network becomes critical.
Recreate Behavioral Health Network provides individualized care designed to meet each person’s unique needs.
Whether you’re just beginning the recovery journey or transitioning from detox to long-term support, you’re not alone. Our experienced team works with you to create a personalized plan, helping you or your loved one regain health, stability, and hope.









